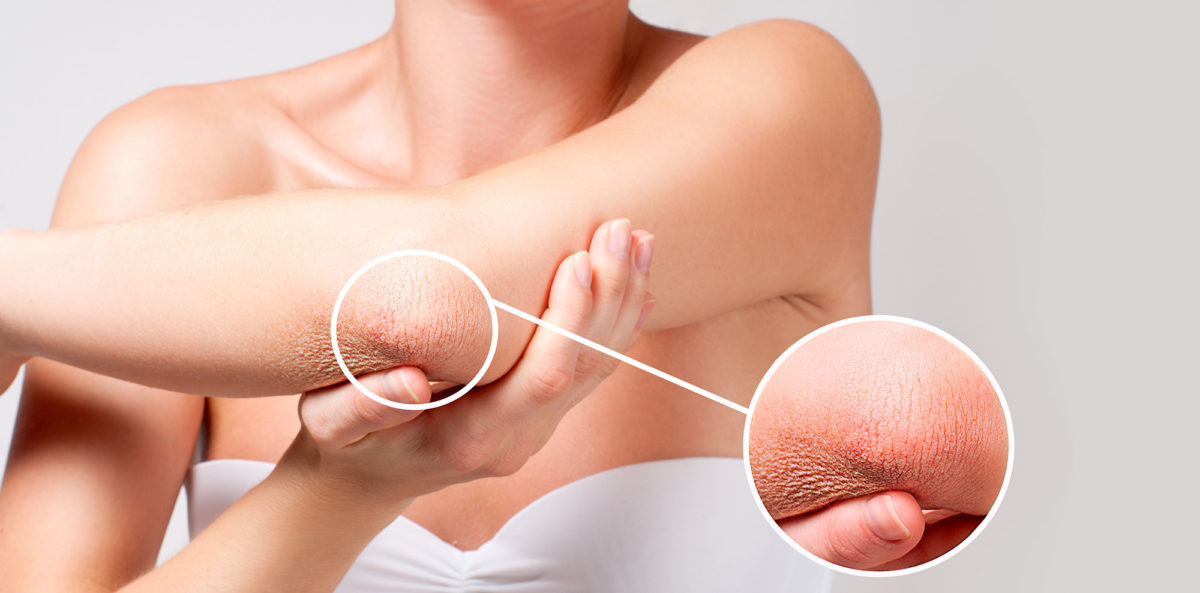
Julie van Onselen, Lecturer Practitioner in Dermatology, Dermatology Education Partnership Ltd, presents an overview of emollients and dry skin conditions, aimed at pharmacists.
Pharmacists are increasingly on the frontline of managing eczema and dry skin conditions. A key component of first-line management is recommendation of the most appropriate emollients, which may be bought over the counter or prescribed. A large retrospective research study examined the patient records of almost 55,000 patients diagnosed with dry skin conditions and eczema, over a four-year period. One group of patients had been prescribed emollients and the other had not. The number of practice visits was significantly lower in the emollient group compared to the non-emollient group. Prescribing an emollient was associated with fewer prescriptions of potent topical corticosteroids.
Whereas patients in the non-emollient group were 18 per cent more likely to require a topical steroid. They were also 13 per cent more likely to require an antimicrobial-containing prescription. (1)
Effects of Dry Skin
Dry skin is synonymous with a skin-barrier defect and is caused by loss of water from the stratum corneum. (2) The primary function of the skin barrier is to restrict water loss and to prevent the entry of irritants, allergens and skin pathogens. When the skin barrier function is impaired, water is lost transcutaneously. Skin dehydration leads to the development of cracks between the skin cells, resulting in inflammation and pruritus. (2)
Several factors may affect the skin barrier function, including ageing, environmental influences like chronic sun exposure, cold, wind, low humidity, chemical exposure, physical trauma, and hormonal changes associated with the menopause. (3)
Dry skin (xerosis) is a common symptom of a number of skin conditions, including atopic dermatitis / eczema (AD/AE), ichthyosis, irritant contact dermatitis, psoriasis and asteatotic eczema. Dry skin can be unsightly and can have a negative impact on a patient’s quality of life through itching, discomfort and embarrassment about their appearance. Left untreated, dry skin can lead to a flare of the underlying condition such as atopic eczema. (2)
Treating Dry Skin with Emollients
The terms emollient and moisturiser are often used interchangeably in the literature. The lack of consistency on the use of these terms can be confusing, especially as many products have both occlusive and moisturising properties. Generally, emollient is used as an inclusive term to describe substances whose main action is ‘to occlude the skin surface and to encourage build-up of water within the stratum corneum’. (4)
Depending on the composition of the emollient, they work either by occlusion, ‘trapping’ moisture into the skin (which slows the evaporation of water), or in an ‘active’ way by drawing moisture into the stratum corneum from the dermis. (5)
A 2013 Consensus Statement recommended that ‘Emollients should be the first line therapy for all dry-skin conditions, including eczema, asteatotic eczema and psoriasis.’ (2) Emollients moisturise the skin by increasing the amount of water held in the stratum corneum. (6)
Emollients help reduce the clinical signs of dryness, such as roughness or scaling, and improve symptoms, like itching and tightness. They need to be cosmetically acceptable to the patient, so they can continue with their day-to-day activities, this will help promote adherence to treatment. (4)
If possible, patients should be given the opportunity to consider a variety of emollients from the wide range of products available, and to identify the most suitable products for their skin. The choice of emollient may be driven by cosmetic acceptability, cream or ointment formulation, oil content, and additional benefits, such as humectant and / or anti-itching properties.
Ideally, an emollient should be prescribed with a pump dispenser to minimise the risk of bacterial contamination. For emollients that come in pots rather than pump dispensers, advise that using a clean spoon or spatula (rather than fingers) to remove the emollient helps to minimise contamination. (7)
Emollients have a steroid-sparing effect and should be supplied in a 10:1 ratio of emollient to steroid in order to achieve the full benefit. (7) Aqueous cream BP should be avoided both as a leave-on emollient and as a washing product. It contains approximately one per cent SLS (sodium lauryl sulfate), an anionic surfactant known to be profoundly irritant. Using Aqueous cream BP weakens the epidermal barrier and increases transepidermal water loss. (2)
Pharmacists are well-placed to give balanced, consistent and accurate advice, and are uniquely equipped to influence care for the better.
Note – this article is based on a National Pharmacy Association-accredited training course ‘Emollients and Dry Skin Conditions’ developed for pharmacists and supported by the Zeroderma range from Thornton and Ross Pharmaceuticals.
The training is available in a series of webinars. Email to register interest and receive further details: zeroderma@thorntonross.com.
About the Author
Julie van Onselen is a Lecturer Practitioner in Dermatology, Director of Dermatology Education Partnership Ltd, which focuses on dermatology educational and service development projects; and independent training. She is a Masters lecturer at the University of Stirling, works clinically one day a week, and also as an adviser for skincare charities.
References
1. Moncrieff, G. et al. (2018) Cost and effectiveness of prescribing emollient therapy for atopic eczema in UK primary care in children and adults: a large retrospective analysis of the Clinical Practice Research Datalink. BMC Dermatology. 18:9
2. Moncrieff, G. et al. (2013). Use of emollients in dry-skin conditions: consensus statement. Clinical and Experimental Dermatology. Vol 38(38), pp. 231–238
3. Monteiro-Riviere, N.A. (2004). Anatomical Factors Affecting Barrier Function https://www.researchgate.net/publication/265225400 accessed 17th June 2020
4. Penzer, R. (2012). Best practice in emollient therapy – A Statement for healthcare professionals. Dermatological Nursing. 11(4), pp1-19
5. Rawlings, A.V., Canestrari, D.A., Dobkowski, B. (2004) Moisturizer technology versus clinical performance. Dermatol Ther 17(Suppl 1): 49–56
6. Cork, M.J. (1997). The importance of skin barrier function. J Dermatol Treat 8: s7–13
7. NICE, CKS https://cks.nice.org.uk/eczema-atopic#!prescribingInfoSub:6 accessed 17th June 2020